Anaesthetic Technician
Kaihangarau Haurehu
Alternative titles for this job
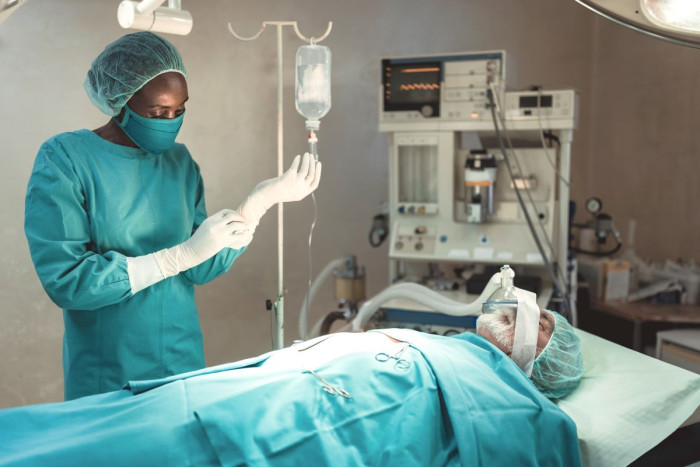
Anaesthetic technicians assist anaesthetists during operations, and prepare operating theatres and clinics for anaesthetic procedures.
Pay
Anaesthetic technicians usually earn
$84K-$99K per year
Anaesthetic technicians can earn
$73K-$105K per year
Source: TEC research
Job opportunities
Pay
Pay for anaesthetic technicians varies depending on experience, hours of work, and employer.
- Anaesthetic technicians usually earn $84,000 to $99,000 a year.
- Anaesthetic technicians can earn $73,000 to $105,000 a year.
Those working in private hospitals usually earn more when they start out.
Source: TEC research.
PAYE.net.nz website - use this calculator to convert pay and salary information
(This information is a guide only. Find out more about the sources of our pay information)
What you will do
Anaesthetic technicians may do some or all of the following:
- check and set up life support and anaesthetic machines
- inform and reassure patients, and check for conditions that could create problems under anaesthesia
- help anaesthetists place patients' breathing tubes and intravenous lines
- help anaesthetists administer anaesthetics, including local anaesthetics and nerve blocks
- watch patients and monitor their vital signs (such as heartbeat)
- decontaminate, sterilise or dispose of equipment and materials used in operations
- assist with care after operations and insert catheters into patients.
Skills and knowledge
Anaesthetic technicians need to have knowledge of:
- operating theatre procedures and protocols
- anaesthetic and nerve-blocking machines, life support machines, other equipment and drugs
- emergency procedures, and how to administer cardiopulmonary resuscitation (CPR)
- human anatomy, physiology and biophysics
- physical and medical conditions that may put patients at risk during anaesthesia.
Working conditions
Anaesthetic technicians:
- usually do shift work, including weekends, and may be on call
- work in operating rooms in hospitals and clinics, delivery suites and emergency departments
- work in conditions that may be stressful, particularly during operations.
Entry requirements
You need a qualification to become an anaesthetic technician.
You need:
- a Bachelor of Health Science (Perioperative Practice)
- to pass a police check
- a CPR certificate.
- Auckland University of Technology (AUT) website - Perioperative Practice major in the Bachelor of Health Science
- New Zealand Anaesthetic Association website - training
The Vulnerable Children Act 2014 means that if you have certain serious convictions, you can’t be employed in a role where you are responsible for, or work alone with, children.
Secondary education
You need University Entrance to do the study or training for this job.
Personal requirements
Anaesthetic technicians need to be:
- able to remain calm in emergencies and work well under pressure
- accurate, with an eye for detail
- good communicators who are able to relate to people from a range of cultures
- comfortable working around sick and injured people.
Useful experience
Experience in the medical field is useful for anaesthetic technicians.
Physical requirements
Anaesthetic technicians need to be reasonably fit, healthy and strong because they often need to move equipment and patients.
Registration
Anaesthetic technicians must be registered with the Medical Sciences Council of New Zealand and hold an Annual Practising Certificate.
Find out more about training
- Auckland University of Technology (AUT)
- 0800 288 864 - www.aut.ac.nz
- New Zealand Anaesthetic Technicians' Society
- nzats@anaesthesia.nz- www.nzats.co.nz
What are the chances of getting a job?
Chances good due to shortage of anaesthetic technicians
Demand for anaesthetic technicians is strong due to:
- New Zealand's growing and ageing population, which means more surgical procedures
- insufficient numbers of trainees.
Anaesthetic technician appears on Immigration New Zealand's regional skill shortage list. This means the Government is actively encouraging skilled anaesthetic technicians from overseas to work in New Zealand.
According to the Medical Sciences Secretariat, 865 registered anaesthetic technicians were eligible to work in New Zealand in March 2021.
Anaesthetic technicians work in hospitals
Anaesthetic technicians work for public or private hospitals.
Sources
- Medical Sciences Secretariat, careers.govt.nz interview, November 2021.
- Immigration New Zealand, 'Regional Skill Shortage List', 27 May 2019, (www.immigration.govt.nz).
- New Zealand Anaesthetic Technicians' Society, careers.govt.nz interview, January 2019.
- New Zealand Anaesthetic Technicians' Society website, accessed January 2019, (www.nzats.co.nz).
(This information is a guide only. Find out more about the sources of our job opportunities information)
Progression and specialisations
Anaesthetic technicians may move into managerial or trainer roles.
Anaesthetic technicians can specialise in certain departments or procedures, including:
- paediatrics (working with children)
- emergency and resuscitation
- transplants
- specialised surgery such as neurosurgery (brain surgery) or cardiothoracic surgery (for heart and lung-related conditions)
- using specialist equipment for cell saving (removing a patient's own blood or blood products, then later returning them to the patient's body).
Last updated 20 November 2024